|
There are two streams in the literature on the economics of obesity. Short-run perspective is one related to the contemporary prevalence of obesity and its associated costs. Long-run perspective looks at the trends in human longevity, and relationship between physical characteristics of the population such as height, weight, or posture and their effect on health and longevity. Although both approaches rely on medical research and other scientific results as their basis, their findings are different. Short-run studies emphasize a strong link between obesity and deteriorating health of the American population and suggest immediate government intervention of various sorts. Long-run studies indicate how obesity and overweight may not be associated with many health problems that short-run studies suggest that they are. This scientific uncertainty leads to a difficult policy dilemma: is obesity a major health problem that demands government attention in terms of health and food policy intervention?
Short-Run Perspective
Several economists have investigated why obesity rates are rising among Americans. According to Lakdawalla and Philipson (2002), the above observed increase in obesity rates in the United States stem from technological change occurring in the last century and have resulted in calories becoming relatively cheaper, while exercise has become relatively more expensive. Individuals have maximized their utility subject to this new budget constraint, and that resulted in higher body mass indexes. Obesity is measured commonly by the body mass index (BMI), which is weight in kilograms divided by height in meters squared. The convention is that overweight people have a BMI above 25, while the obese people have a BMI above 30 (Figure 1). Cutler, Glaeser, and Shapiro (2003) point out that, according to the standard economic model, the resulting obesity is not necessarily viewed as a bad outcome. People make choices and if they choose to eat more and exercise less in the face of the current environment and circumstances, it must be because that makes them happier than eating less and exercising more. The implication of this simple economic analysis is that there is no reason to intervene with policies to reduce obesity, since it is merely the outcome of individuals pursuing their own self-interest.
There are, however, several reasons why one should not endorse the standard economic model's laissez-faire implications when it comes to obesity. First, the standard economic model requires well-informed individuals who are free to make their own choices. We have already seen that a large number of children in the United States are either obese or overweight. Children, generally speaking, rarely purchase their own food or determine what is for lunch or dinner either at home or at school (Anderson, Butcher, and Levine, 2003).
Second, if overweight and obese people consume more medical care, and if much of that medical care is paid for by society rather than the individual, then there is a negative externality associated with high rates of being overweight or obese. In 2000, the direct costs to society of obesity-related disease were estimated at $61 billion, while indirect costs to society were estimated at $56 billion (Cutler, Glaeser, and Shapiro, 2003). Direct costs include healthcare expenses such as physician visits and hospitalizations. Indirect costs are the value of lost wages by those who cannot work due to sickness or disability and foregone earnings attributed to premature death resulting from obesity or being overweight.
Finally, Cutler, Glaeser, and Shapiro (2003) argue there might be internalities or costs borne by individuals themselves because of their higher weights. These internalities exist in the presence of self-control or addiction problems: people would like to eat less than they do, but have difficulty limiting their consumption. They are similar to externalities because they result from individuals when they are consuming food, not internalizing the impact on their future happiness.
Economists may care about policy interventions to address obesity for at least one more reason. The government already intervenes in people's lives in many ways that may have intentional or unintentional consequences for their weight. Public spending on transportation or parks, for instance, may affect the amount of exercise people get. The USDA's Food Guide Pyramid (2005) provides the government's definition of a healthful diet. This, in turn, affects the food that schools serve to children. Education policies affect physical education requirements in schools. Also, economic and social policies may have direct or indirect effects on parents' labor supply, thus potentially affecting the amount of time they have to oversee their children's diet and exercise.
Long-Run Perspective
Painting an accurate picture of the health of past populations can help us assess trends in living standards, forecast future mortality rates, and understand long-run implications of any new food policy measures. Many of the short-run studies on possible obesity prevention policies presuppose a non-zero, and often large, benefit from reducing obesity rates in the population, which stems from improved health and decreased morbidity. Yet, none of these studies looked into the long-term health trends and the role that overweight and obesity play in them. A different stream of literature emerged researching this issue. Findings from these studies certainly challenge results and policy suggestions coming from some of the short-term studies.
Several studies have analyzed long-term health trends using the Gould sample. This longitudinal data set contains age, physical and health characteristics of 23,785 Union soldiers in the1860s, 1880s, and early 1900s. These studies also used comparable data sets from the U.S. Army from the 20th Century. Analysis of the Gould data set reveals that past populations were shorter-lived, smaller, lighter, and faced a heavier disease burden in old age (Costa, 2004). The BMI's of Union soldiers were found to be 23 on average compared to a BMI of 26 for modern U.S. Army soldiers (Costa and Steckel, 1997). However, these authors as well as Fogel (2005) focus not only on BMI as a health indicator but on seven anthropometric indicators: height (an indicator of frame size), BMI (a measure of total body fat), waist-hip ratio, the ratio of chest circumference to shoulder breadth, the ratio of chest circumference to height (all indicators of central body fat), lifting strength (an indicator of muscle strength), and vital capacity (a measure of lung capacity), and a number of socio-economic and demographic variables. Their findings are that there have been substantial changes in the human frame over the last hundred years as men have become taller and heavier. Controlling for total body fat, men today have less abdominal fat than the past populations.
This type of fat patterning predicts hypertension and ischemic and cerebrovascular disease in modern populations and predicted death from ischemic and cerebrovascular disease in a past population where cause of death information is relatively rare. The findings indicate that these diseases were present in this past population and may have even been as prevalent as they are today. Although infectious and parasitic diseases were highly visible in the past and considered the main cause of mortality, the burden of "modern" chronic disease was still there. For instance, Fogel (2005) found that the average age of onset of chronic heart conditions among American males near the beginning of the 20th Century was 55.9 years of age and near the end of the 20th Century was 65.4 years of age. This burden, however, was not evenly distributed. Examining the seven anthropometric indicators listed above showed that in the mid-19th Century, populations who were at greater risk of developing modern chronic diseases included the foreign born and large city dwellers. Henderson (2005) also used Gould sample data in his analysis and compared it with data from the first National Health and Nutrition Examination Survey (NHANES I) conducted between 1971 and 1975. His results indicate that the frontiers of overweight and obesity are expanding over time, such that the potential risk is today associated with higher levels of BMI. Results consistent with this study are found in Flegal et al. (2005) who conclude that being overweight may not be significantly associated with excess mortality and the risk of obesity on mortality may have decreased.
The theory of technophysio evolution was recently introduced to explain the changes in human appearance during the last 300 years and in particular during the last century (e.g., Fogel and Costa, 1997; Fogel, 2005), unlike the genetic theory of evolution through natural selection that applies to the whole history of life on earth. The theory of technophysio evolution is based on the proposition that during the last 300 years (and especially during the last century), human beings have gained an unprecedented degree of control over their environment that set them apart not only from all other species, but also from all previous generations of Homo sapiens. This new degree of control has enabled Homo sapiens to increase their average body size by over 50 percent, to increase their average longevity more than 100%, and to greatly improve the robustness and capacity of their vital organ systems (Fogel, 2005). Advances in the technology of food production after the second Agricultural Revolution (which began about 1700), in combination with new technological advances in manufacturing, trade, transportation, energy production, communications, or medical research and services, are believed to be responsible for the observed changes in average longevity and body size. However, evaluating which environmental factors have contributed the most to the observed declines in morbidity and mortality remains an active research agenda.
Obesity and Overweight: Policy Dilemma
A change in trends in obesity in the United States that occurred in the last 20 years has obviously left scientists in medical research undecided at the moment about the actual effect this epidemic may have or already has on the health and mortality rate of the American population. Indeed, what we seem to have learned from the studies using longitudinal data is that previous populations, albeit having significantly lesser BMI than today's population, suffered from the same chronic diseases that are commonly thought to be caused by being overweight and obese. If the government is to be called into action to stop or reverse this obesity trend, that may not be solely in order to improve the health of the population, but also to protect current standards on how the population should look or because weight reduction and health protection are erroneously being equated. From a purely health policy point of view, most of the larger health concerns were handled in the past and obesity seems to be the issue we seem to want to address now. However, just because this issue is on the top of the hierarchy now we need to recognize that 'solving' it may not have the kind of impact that was associated with solving some of society's earlier health issues and needs (e.g., penicillin, war on malaria).
Even if the motives behind any potential government intervention in this matter may be most noble, it is clear that the entire economy would be greatly affected by these policies. And any government intervention will produce winners and losers with both net social gains and losses being plausible outcomes. For example, current guidelines recommend increased consumption of fruits, vegetables, fish, and whole grains, within the context of a diet whose overall calories have been moderately reduced. While this diet, if implemented on a large scale for a sustained period of time, is likely to benefit producers in these industries, reduced consumption of other foods such as meats, dairy, or sugar, to name a few, would force many producers out of business or greatly reduce their profit margins.
For More Information
Anderson, P.M., Butcher, K.F., & Levine, P.B. (2003). Economic perspectives on childhood obesity. Economic Perspectives, 3Q, Federal Reserve Bank of Chicago.
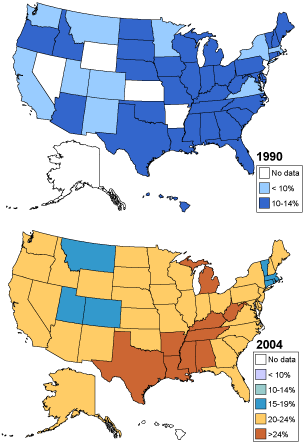
Behavioral Risk Factor Surveillance System. (1990, 2004). National Center for Chronic Disease Prevention and Health Promotion, Center for Disease Control. Available online: http://www.cdc.gov/brfss/.
Costa, D.L. (2004). The measure of man and older age mortality: Evidence from Gould sample. Journal of Economic History, 64(1), 1-23.
Costa, D.L., & Steckel, R.H. (1997). Long-term trends in health, welfare, and economics growth in the United States. In R. Floud and R.H. Steckel (Eds.), Health and Welfare during Industrialization. Chicago: University of Chicago Press.
Cutler, D.M., Glaeser, E.L., & Shapiro, J.M. (2003). Why Have Americans Become More Obese? Harvard Institute of Economic Research, Discussion Paper No. 1994, January, Cambridge, MA: Harvard University. Available online: http://post.economics.harvard.edu/hier/2003papers/HIER1994.pdf.
Flegal, K.M., Graubard, B.I., Williamson, D.F., & Gail, M.H. (2005). Excess deaths associated with underweight, overweight, and obesity. Journal of American Medical Association, 293, 1861-1867.
Fogel, R.W. (2005). Changes in the disparities in chronic diseases during the course of the 20th Century. Perspectives in Biology and Medicine, 48(1), S150-S165.
Fogel, R.W., & Costa, D.L. (1997). A theory of technophysio evolution, with some implications for forecasting population, health care costs, and pension costs. Demography, 34(1):49-66.
Henderson, R.M. (2005). The Bigger the healthier: Are the limits of BMI risk changing over time? Economics & Human Biology, 3(3), 339-366.
Lakdawalla, D., & Philipson, T. (2002). The growth of obesity and technological change: A theoretical and empirical examination. NBER Working Paper No. 8946.
U.S. Department of Agriculture (USDA). (April 2005). Food Guide Pyramid. Washington, DC: Center for Nutrition Policy and Promotion. Available online: http://www.mypyramid.gov/.
|
|