For decades, from the 1940s to the 1970s, the goal of U.S. food and nutrition assistance programs seemed clear: to make sure low-income Americans could afford enough food. By pursuing this goal, the programs would protect program participants from hunger and also support demand for farm products. Today, about one in five Americans receives benefits from at least one of the U.S. Department of Agriculture’s (USDA) food programs. The major programs include the Supplemental Nutrition Assistance Program (SNAP), Special Supplemental Nutrition Program for Women, Infants, and Children (WIC), school meals programs—lunch and breakfast, and the Child and Adult Care Food Program. Despite the food programs’ goal of reducing hunger and improving nutrition, rising concern about overweight and obesity for all Americans has triggered arguments that targeted food benefits could be counter-productive. As a recent retrospective on a century of food and consumer economics explained, “The policy context for food assistance programs has changed in the past three decades.” (Unnevehr et al. 2010, p. 512).
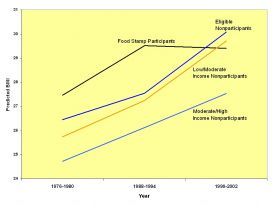
This policy context has motivated new research about how food assistance programs affect body weight and the risk of overweight. For example, a recent USDA study compared women who participated in the Supplemental Nutrition Assistance Program (SNAP)—the new name for the Food Stamp Program—to low-income nonparticipants (Ver Ploeg and Ralston, 2008) (Figure 1). From the 1970s to the 1990s, Non-Hispanic White women who participated in SNAP had higher weights, hinting—but by no means proving—that the program had unintended consequences for weight status. In the 1990s, by contrast, the gap between participants and nonparticipants disappeared. Unfortunately, this disappearance is not as much good news as you might think. The gap disappeared because nonparticipants gained weight faster in the 1990s, reaching the same high weights that SNAP participants had on average.
It is well known that such comparisons of participants and nonparticipants provide only limited information about real program effects. There are many plausible interpretations of a weight gap between participants and nonparticipants. People with higher weights may be more likely to participate in food assistance programs for other reasons, such as giving a higher priority to food or having poorer health.
To some extent, this problem of multiple interpretations can be addressed with more advanced statistical analyses. Several studies over the years, using diverse methods, have suggested that participation in SNAP appears to increase the risk of obesity, at least for women, even when one controls as well as possible for other confounding factors (Gibson, 2003; Meyerhoefer and Pylypchuk, 2008). Yet, it remains very difficult to demonstrate directly that food assistance programs either do or do not raise the overall risk of overweight and obesity.
To understand the potential effects of food assistance programs, it is useful to take a closer look at what the programs actually do. Experts have reached widely different conclusions about the effect of food assistance programs on ultimate health outcomes in part because they give different levels of emphasis to the diverse activities that food assistance programs carry out. To take just one example, if you think of food assistance programs mainly as a way to increase total food intake, you may be more worried about the effect on obesity. On the other hand, if you think of food assistance programs mainly as a way of assuring a reliable and steady source of food, less subject to the “boom and bust” cycles of hunger and food insecurity, you may be more optimistic that the programs will reduce the risk of obesity.
Consider the following five major activities of food assistance programs, which could affect weight status in surprisingly diverse ways, both favorable and unfavorable. The research literature has long studied some of these program activities, while research on others has just begun.
SNAP benefits per participant per month in 2009 averaged $124, which must by law be spent only on eligible food and beverages from authorized retailers. Of course, the participants would have had to spend money on food even in the absence of the program, so not all of these SNAP benefits represent an additional increase in food spending. Assuming that 20% of the benefits are truly additional, beyond what would have occurred anyway, the program increased food expenditures by about $25 per person per month on average. The WIC program provides a package of supplementary foods to eligible low-income women, infants, and young children. The levels and types of foods are chosen to enhance the amount of available foods and nutrients consistent with current scientific evidence. School-age children from low-income families are eligible for free or reduced price meals through the National School Lunch Program and School Breakfast Program.
These programs substantially increase the total food resources available to low-income families. The proportional impact on actual food intake in terms of food energy—calories—is much smaller, because the increased food resources allow families to prioritize many aspects of food quality and desirability beyond just quantity of calories. Nevertheless, either explicitly or implicitly, the argument that food assistance programs contribute to obesity usually hinges on the belief that these additional food resources may in combination be more than participants need to maintain energy balance.
Many food assistance programs are accompanied by rules or restrictions about what foods can be purchased or acquired through the program. The WIC program, for example, specifies quite narrowly the package of items that may be included, based on the pregnancy status and breastfeeding practice of mothers, and on the age of the infant or child. Originally, the foods in the package were chosen specifically because of the extra protein and a limited set of target micronutrients they provide. More recently, the package has been revised to consider the problem of over-nutrition as well as under-nutrition. For example, the amount of fruit juice and cheese has been reduced, the type of milk is restricted to low fat or skim milk for participants over one year old, and a new fruit and vegetable benefit has been added.
The school meals programs, similarly, include a requirement that links the meal menus to the federal government’s Dietary Guidelines for Americans. However, the requirements are currently loose enough that an active debate continues about the role of these programs during this period of rising rates of childhood obesity (Ralston et al. 2008). New recommendations under consideration would require offering foods that have reduced saturated fat, are low in sodium, are rich in whole grains and include a variety of fruits and vegetables (Institute of Medicine, 2009). At the same time, calories offered would need to fall within a minimum/maximum range determined by age. Current regulations specify a minimum level of calories offered.
SNAP, by contrast, is sometimes described as if it provides no constraints on the healthfulness of the foods that can be purchased. Cigarettes and alcohol are forbidden, along with paper goods and other non-food products, but otherwise most foods and beverages in the grocery store are eligible. Early research found that program benefits were associated with increased consumption of discretionary fats and added sugars, but not significantly increased consumption of fruits and vegetables (Ver Ploeg and Ralston, 2008). While some have proposed that SNAP benefits could be restricted to a narrower list of foods, these proposals have not been able to overcome the concern that making the program more restrictive would discourage participation by eligible low-income people. SNAP does have one important food restriction, which has received more attention recently. Because the program benefits are restricted to foods that are intended for consumption at home—or at least off the retailer’s premises—SNAP tends to increase grocery purchases at the expense of restaurant or away-from-home purchases (Wilde, Troy, and Rogers, 2009).
Nutrition education has long been a central component of the WIC program and is a required part of WIC services. Although the main activity of SNAP is to provide benefits to support food purchases, nutrition education has become an increasingly important secondary activity in state SNAP agencies. In this voluntary component of SNAP, states may propose a nutrition education plan to the federal government. Federal and state governments share the costs approximately equally. The federal contribution to nutrition education for SNAP participants grew from less than $1 million in 1992 to more than $270 million in 2007. In its guidance for state agencies conducting nutrition education, USDA’s Food and Nutrition Service focuses on promoting specific behaviors, such as increased physical activity and increased fruit and vegetable consumption, which are associated with lower risk of obesity. Nutrition education offered through school programs in Team Nutrition and increased availability of fruits and vegetables in the school setting are designed to increase exposure to a variety of foods, promote healthy eating and, ultimately have an effect on reduced weight.
Food assistance programs may affect food markets in ways that have implications for all low-income consumers, participants and nonparticipants alike. The WIC program, for example, has a small farmer’s market promotion program, which is designed in part to encourage healthful alternative retail options in low-income communities. Beyond these newer and small-scale efforts, the WIC purchases and rebates from infant formula manufacturers have the potential to increase the price of formula faced by non-WIC participants (Oliveira et al. 2005). Until recent changes in program benefits and formula rebates, the relative price difference in infant formula meant that the program benefit with formula feeding outweighed the program benefit received by nursing mothers and encouraged early use of formula feeding. Infant feeding practices that include increased practice and duration of breastfeeding are associated with reduced risk of illness and excessive weight gain later in childhood.
Other large food assistance programs, such as SNAP, operate on a large enough scale they could influence the overall economic viability of full-service grocery retailers in low-income neighborhoods. Recent research contemplated more specifically the possible effects of SNAP policy changes on agricultural markets. Alston et al. (2009) investigate whether restricting SNAP benefits to comparatively healthy products could increase the price of those products, thereby affecting the purchases of low-income nonparticipants. Alternatively, expanding the market for these products and increasing market access may increase their availability in some low-income markets.
Food assistance program participants tend to have higher rates of food insecurity and hunger than seemingly similar nonparticipants do. This finding has sometimes been called a “paradox,” but it should not really be surprising. People who face greater concerns with food insecurity and hunger are more likely to undertake the effort to participate in food assistance programs. Recent research has intensified the effort to control for this type of self-selection, in order to measure the real effects of program participation. For example, Huffman and Jensen (2008) found that when one controlled as well as possible for self-selection, it no longer appeared that SNAP participants had higher rates of food insecurity.
The relationship between SNAP participation, food insecurity, and obesity is complex. Women in moderately food insecure households tend to have higher weights on average than women in food secure households. Results are less clear for men. The reason for this pattern is not entirely clear, though being food insecure may be related to "boom and bust" cycles in food intake, which could be related to weight gain.
Alternatively, being food insecure may require households to sacrifice healthy food choices in favor of less expensive and more fattening sources of calories. Or, some other characteristic of food insecure households, such as increased stress or reduced time for physical activity, may also be related to higher weights. SNAP participation might help in some ways to ameliorate this problem, by providing a reliable source of economic resources for food purchases. However, SNAP benefits received only once per month are typically exhausted or nearly exhausted long before the end of the month—the boom and bust cycle. It would be worthwhile to test more frequent benefit delivery, on a pilot basis, to see if this change protects participants from sporadic food insecurity and improves the healthfulness of food purchases late in the month.
Food assistance programs do more than just provide food. They may increase resources for food spending, while at the same time providing nutrition education. They may limit purchases or regulate reimbursable foods and meals in ways that reduce the potential impact on weight gain. They may encourage healthy eating practices among children and have longer term consequences on improving food choices. They may influence food prices and food retail access in low-income neighborhoods. They may ameliorate food insecurity, or at least target resources toward the needs of people who are particularly at risk of food insecurity.
Determining whether food assistance programs have a direct or indirect effect on obesity is a complex issue. Many factors, both diet, physical, and contextual can influence the health outcome. Public programs have an opportunity to affect eating behaviors in a wide variety of ways, and at different times in the lives of participants. As new evidence emerges on food choices and eating behaviors that contribute to obesity, USDA is challenged to incorporate the evidence in designing programs that both promote healthy food choice and, at the same time, support efforts to ameliorate hunger. Despite the complexity, the challenge encourages research designed to focus more closely on the programs’ distinct goals and activities in a way that actually provides more useful information for thinking about policy improvements.
Alston, J.M., Mullally, C.C., Sumner, D.A., Townsend, M., Vosti, S.A. (2009). Likely effects on obesity from proposed changes to the US Food Stamp Program. Food Policy, 34, 176-184.
Gibson, D. (2003). Food stamp program participation is positively related to obesity in low income women. Journal of Nutrition, 133, 2225-2231.
Huffman, S. K., and Jensen, H.H. (2008). Food assistance programs and outcomes in the context of welfare reform. Social Science Quarterly, 89(1), 95-115.
Institute of Medicine. (2009). School meals: Building blocks for healthy children. Washington, D.C.: Food and Nutrition Board, Institute of Medicine, National Academies.
Meyerhoefer, C., and Pylypchuk, Y. (2008). Does participation in the food stamp program affect the prevalence of obesity and health care spending? American Journal of Agricultural Economics, 90(2), 287-305.
Oliveira, V., Prell, M., Smallwood, D., and Frazao, E. (2005). WIC and the retail price of infant formula. FANRP Report 1. Washington, D.C.: U.S. Department of Agriculture, Economic Research Service.
Ralston, K., Newman, C., Clauson, A., Guthrie, J., and Buzby, J. (2008). The national school lunch program background, trends, and issues. Economic Research Report 61. Washington, D.C.: U.S. Department of Agriculture, Economic Research Service.
Unnevehr, L., Eales, J., Jensen, H.H., Lusk, J., McCluskey, J., and Kinsey, J. (2010). Food and consumer economics. American Journal of Agricultural Economics, 92(2), 506–521.
Ver Ploeg, M., Mancino, L., and Lin, B.-H. (2006). Food stamps and obesity: Ironic twist or complex puzzle? Amber Waves, 4(1), 32-37.
Ver Ploeg, M., and Ralston, K. (2008). Food stamps and obesity: What do we know? Economic Information Bulletin 34. Washington, D.C.: U.S. Department of Agriculture, Economic Research Service.
Wilde, P.E., Troy, L.M., and Rogers, B.L. (2009). Food stamps and food spending: An Engel function approach. American Journal of Agricultural Economics, 91(2), 416-430.